Our hospital is in difficulty. There is no getting around it.

A Zen insight my teacher once shared is as our meditative practice deepens, our ability to hear the cries of the world also grows. Hearing those cries our deep bodhicitta (heart of love) is touched and (in time) leaves us with little choice but to respond.
It seems that time may have come for me. Hearing the cries of my hospital, sometimes literally in its corridors, I put myself forward recently to take on a new role, well outside my traditional boundaries. The interview was last week and here is a brief summary of what I presented.

I started with where we were as a hospital. This was straightforward enough. Four different reports (three within the last year) make clear beyond argument how difficult the current situation is. Yet a report can at best only touch the surface of what is happening. To understand the real human suffering underlying any report we must be able to open our hearts with compassion and courage.
Embracing the suffering, instead of denying it or finding someone to blame, opens not only our hearts but also our minds. It creates the space where we can explore why and learn from it – strengthening the roots of understanding of what can be and how to get there – in a partnership of equals.
For me, I have the aspiration of seeing our hospital become a high reliability organisation. Where at any moment thousands of errors could happen but don’t. A system and culture that have been nurtured in a way to prevent potential catastrophes from manifesting. In a word, an organisation that has developed its own “collective mindfulness”.
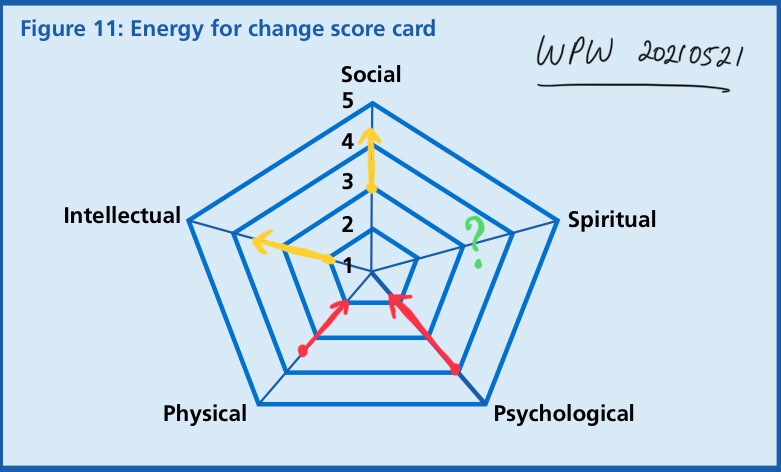
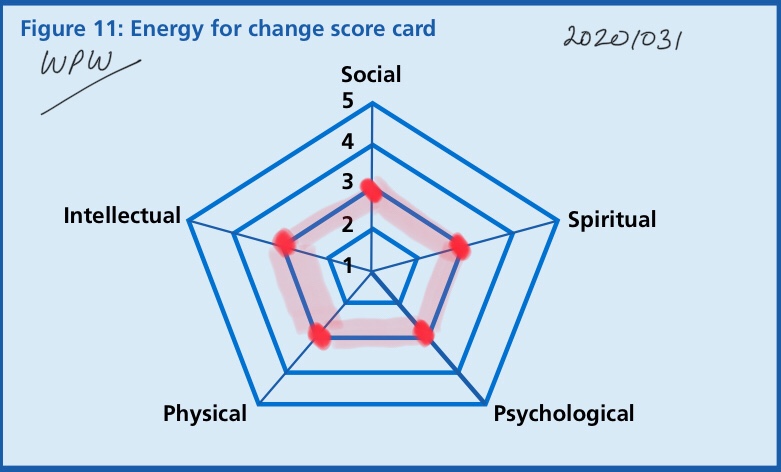
Where does an organisation find the energy to do this ? The literature on large scale change provides a clear answer – there are five sources and each of them play a crucial part in the journey.
Nurturing and directing these energies require a different kind of leadership as well – technically referred to as “ambidextrous”. Where we use both our logical and our creative human strengths to let our best selves shine – as an individual and as an organisation.

The journey is not easy. Even more difficult might be acknowledging the harsh reality of how our hospital reached this moment and facing this with honesty, hope and patience. Yet only by doing so can we give birth to the foundation of a compassionate culture, a clarity of systems and a loving community.
I closed with a message of hope and the belief in a future our hospital could move towards. In the words of Nobel laureate Rabindranath Tagore, (a hospital) where the mind is without fear, and the head is held high …
The decision now lies in the hands of a chosen four. Regardless of the outcome, my personal aspiration is to continue growing a heart of love and finding skilful ways it can express itself in my community.
- Images – Canva
- Reference links: Leading Large Scale Change; High Reliability Organisations